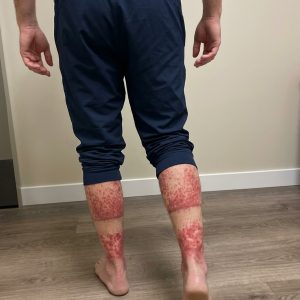
Psoriasis is a chronic skin condition that affects millions of people and goes far beyond a simple rash or temporary irritation. It is an immune-related disorder in which the body accelerates the production of skin cells, causing them to build up rapidly on the surface. This results in thick, inflamed patches that are often covered with silvery scales. These areas can appear on various parts of the body, most commonly the elbows, knees, scalp, and lower back, but they may also affect the hands, feet, and nails. One important fact is that psoriasis is not contagious, meaning it cannot be spread through touch or close contact. Instead, it develops due to a combination of genetic factors, immune system dysfunction, and environmental triggers. Living with psoriasis involves managing both the physical symptoms and the emotional impact that can come with a visible, long-term condition.
There are several forms of psoriasis, each with its own characteristics. The most common type is plaque psoriasis, which appears as raised, red patches with white scaling and may cause itching or discomfort. These patches can come and go in cycles, sometimes improving and then returning unexpectedly. Another form, guttate psoriasis, often develops suddenly, especially after infections, and appears as small, drop-like spots scattered across the body. It is more common in younger individuals and may resolve on its own or develop into a more persistent form. Pustular psoriasis is less common but more intense, involving red skin covered with white, pus-filled blisters that can be painful and sometimes accompanied by fever or fatigue. Inverse psoriasis affects skin folds, such as under the arms or in the groin, where the skin appears smooth, red, and irritated rather than scaly. The most severe form, erythrodermic psoriasis, involves widespread redness and peeling over large areas of the body and requires urgent medical care due to potential complications.
The causes of psoriasis are complex and involve an overactive immune response. In this condition, immune cells mistakenly attack healthy skin, speeding up the life cycle of skin cells and leading to buildup. Genetics play a significant role, as people with a family history are more likely to develop it. Environmental triggers can also cause flare-ups, including stress, infections, cold weather, smoking, alcohol consumption, and certain medications. These triggers vary from person to person, making the condition unpredictable at times.
Diagnosis is usually based on a physical examination, where a healthcare provider identifies the typical appearance and distribution of lesions. In some cases, a small skin sample may be taken to confirm the diagnosis. Nail changes, such as pitting or discoloration, can also provide useful clues. Although there is no cure, many treatments are available to control symptoms. These include topical creams to reduce inflammation, light therapy, and medications that regulate the immune system in more severe cases.
Managing psoriasis also involves lifestyle choices such as maintaining skin hydration, reducing stress, and avoiding known triggers. The condition can affect confidence and daily life, but with proper care and awareness, it can be effectively controlled. People with psoriasis can live full and active lives, focusing on overall well-being while keeping symptoms manageable.